Understanding these cost-sharing terms and how they apply to your healthcare plan can help you plan for healthcare expenses. It can also help you make decisions about the best type of plan for you.
Deductible
A deductible is the amount you’re responsible for before your plan starts to help cover expenses. Only the care you receive while staying in your provider network counts toward your deductible. Once you meet your deductible, your plan starts paying part of your healthcare costs.
Coinsurance
Coinsurance is your share of the cost of a healthcare service. It’s a percentage of the amount charged for services. You start paying coinsurance after you’ve paid your plan’s deductible.
Copay
This is the fixed amount that you pay for a covered healthcare service.
Out-of-pocket maximum (OOP maximum)
The OOP maximum is the most you could pay in a year for covered services. After you meet the maximum amount, the plan will usually pay 100% of the allowed amount. (The allowed amount is benefit payments for covered services based on the amount of the provider’s charge that we recognize for payment of benefits.) If you have other family members in this plan, the overall family out-of-pocket maximum must be met.
Let’s imagine your plan has the following in-network benefits:
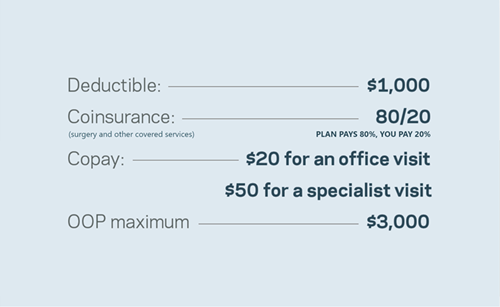
Now, let’s say you receive the following care after breaking your ankle:
- Visit to an orthopedic specialist
- Ankle fracture repair surgery

Now you’ve met your out-of-pocket maximum of $3000 for the year. So, if you need further care this year, your plan will usually pay for all covered care with no additional cost to you for the remainder of the year.
Your actual healthcare costs might not look like this, but knowing how your plan’s cost-sharing works can help you plan ahead.
Benefits are subject to the terms, limitations and conditions of your plan. Please refer to your benefit booklet for a complete listing of your plan benefits.

